When you have elderly relatives, the current images of ambulances waiting for hours on end outside hospitals are particularly worrying. Add on days with strike action meaning only ‘category one’ calls to 999 can be guaranteed an ambulance – how are we meant to sleep at night?
Two scary statistics for you:
- Half of those over 65 have two or more health conditions and
- They are responsible for over 2/3 of hospital admissions.
(Source: https://www.ndph.ox.ac.uk/)
Malnutrition and the NHS crisis
While fixing the NHS crisis might be out of our hands, one thing we can do is keep our elderly generation stronger for longer. This will help the NHS and also our loved ones. There are so many reasons why we must address the issue of malnutrition in the elderly.
1 in 10 people over 65 in the UK is at risk of malnutrition. Malnutrition causes frailty, and susceptibility to disease and slows recovery from wounds and injury.
Why is good nutrition for the elderly SO important?
It’s simple really:
a well-nourished older generation will be less susceptible to falling over or becoming ill.
Fewer elderly people breaking bones and falling ill means fewer ambulances being called leaving more ambulances available to attend crisis calls.
Fewer elderly people breaking bones and falling ill means fewer people stuck in hospital beds leaving more available on wards. – patients can move out of A&E and ambulances can hand over their patients more quickly.
How can we stay stronger in old age?
There are some simple things we can all do to help our elderly relatives and ourselves as we age.
- Use full-fat milk instead of semi-skimmed.
- Eat High protein foods like red meat, oily fish and nuts. These help heal wounds.
- Eat gentle fibre such as oats to keep your bowels moving.
- Eating little and often is best and swapping biscuits and cakes for healthier snacks can really help.
Preventing Frailty Will Help To Fix Our Broken NHS
Why is our NHS at breaking point? Well, lots of reasons…..so I’ll try to sum it up without being too political!
- Strangely, advances in medicine Research and new technology cost money. This research and technology mean that the population are living longer. Both improved health care and an ageing population are expensive.
Traditionally to help the health service cope with this demand, the NHS budget has risen by 4% over inflation every year. However, since 2010 the average rate of increase has been half that. (Source: https://www.nhsconfed.org/articles/is-nhs-awash-with-cash)
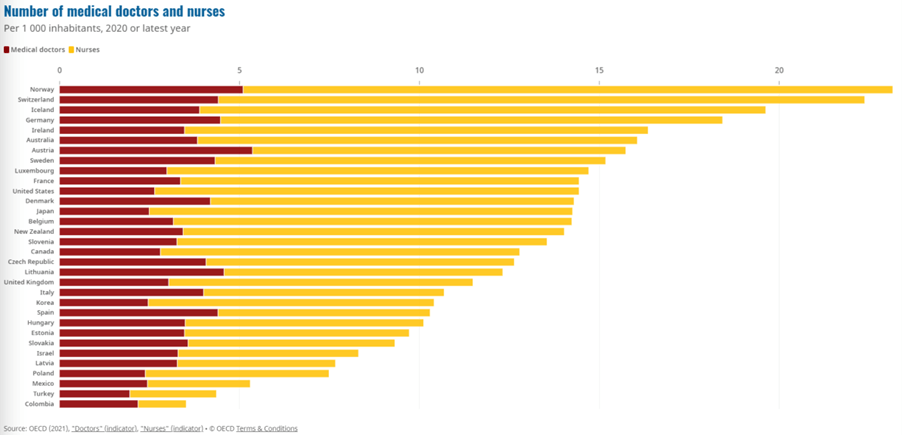
- This spending squeeze has put more pressure on staff across the NHS and there are now fewer doctors and nurses per 1000 population than previously and than most countries in the OECD.
Pay for NHS staff has also been cut over the last decade once inflation has been taken into account so people are leaving in droves. This is causing stress and greater workloads for hospital staff, also meaning many will get sick themselves.
These two points mean there are more patients being treated by fewer medical staff who have lower real budgets for the treatment.
Social Care
This has been a problem since the creation of the NHS 70 years ago. The NHS is funded nationally, while social care has always been the responsibility of local councils. Cottage hospitals and sanitoria have all but been closed, meaning there are no ‘halfway houses’ left between the hospital and going home. Many people cannot afford to pay for private carers at home, but the criteria for funded care are narrow and only met by the very poor and very ill.
Pay for carers is very low, despite long and unsociable hours as well as a great responsibility for the vulnerable. Therefore, this sector is extremely understaffed, causing many care and nursing homes to close or take fewer residents. Agencies that provide carers in people’s own homes are also struggling to recruit and retain staff.
And so we come to……
Bed Blocking
Bed blocking is why ambulances struggle to ‘offload’ patients to A&E.
A&E is full…..due to wards being full…..because many of the elderly can’t leave hospital to go home without carers provided by Social Care. To reiterate: the elderly (over 65s) takes up 2/3 of the hospital beds.
Written by Mary Merheim
BSc (Hons)
Nutrition Advisor for the Elderly
Dementia and End of Life Doula.
Mary Merheim initially created Grandbars in 2018 to keep her father eating when his appetite waned. After much development, research and investment Grandbars was launched in June 2022. They are delicious, nutritious and easy-to-eat no-bake mini cakes.
Use this link to get 20% off your first order at
Additional Sources
BBC News 12.01.23